From Healthcare Employee Engagement to Patient Satisfaction: Your Guide to Building a Service-Value Chain
Follow these six steps to increase healthcare employee engagement and improve patient satisfaction. Learn more here.

Back in 1747 Scottish physician James Lind finally put an end to the age-old “what-treats-scurvy” debate: is it cider? seawater? vinegar?
He found 12 scurvy-inflicted sailors, conducted one of the first ever clinical experiments in the history of medicine…. and confirmed that two oranges and one lemon would do the trick. This marked the beginning of evidence-based health interventions, now a cornerstone of modern medicine.
Today the use of evidence within the healthcare industry has evolved to include a relatively new area: employee engagement.
Meaningful employee engagement — a key driver of healthcare quality — is now a critical issue. In the US, hospitals no longer have access to an open checkbook. Since 2012, under the Affordable Care Act (ACA), the federal government has considered patient satisfaction surveys when determining hospital reimbursement levels. More recently, it has started boiling down patient feedback into a five-star rating, making it easier for consumers to use information on the Hospital Compare website. The bottom line? If patients are not satisfied, healthcare organizations earn less money.
Short of putting a chocolate on patient beds every night, what’s a hospital to do? The clear answer is to boost patient satisfaction through evidence-based HR programs that support, develop, and enable committed, skilled workers.
Healthcare’s Service-Value Chain Defined
Healthcare organizations need look no farther than the likes of Southwest Airlines and Zappos for examples. These businesses have recognized that an engaged workforce leads to productivity, which leads to happy customers, which in turn leads to revenue growth and profitability.
Called the “Service-Profit Chain,” these are all links in the operating strategy and service delivery system of successful customer-centric businesses. In healthcare, this is the “Service-Value Chain,” linking employee commitment and dedication to a better patient experience.
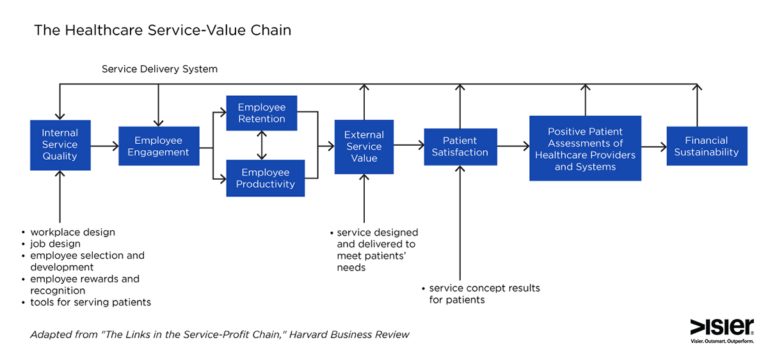
Six Steps Towards Meaningful Healthcare Employee Engagement
If you work in healthcare HR, the following six steps are for you. Use these to master the Service-Value Chain and proactively address workforce issues impacting patient satisfaction — before your hospital suffers a reduced star rating:
Step 1. Gather Employee Engagement Data
Start by gathering all the data from your employee engagement surveys. Break down the engagement score into categories, such as work environment, rewards, and supervisor experience. The more often the employee population has been surveyed, the more timely and relevant the insight will be, so consider moving away from once-a-year engagement surveys to shorter pulse surveys.
Step 2. Gather Patient Experience Data
Make sure you have all of the available patient satisfaction data on-hand. A patient experience measurement, performance analytics and strategic advisory solution, such as Press Ganey Insight, uses well known measures such as the Net Promoter Score to reveal how satisfied patients are with the service they receive.
Step 3. Align the Data
Align the structure of employee engagement data to your patient experience data. This involves matching the structure used to capture the customer data (ward or clinical area), with the structure used to capture the employee engagement data (shift or clinical work group). Some modern workforce technologies will support you to make this mapping process relatively straightforward.
Step 4. Look for connections and correlations
Look for relationships between employee engagement and patient experience scores, such as a low NPS or low speed of service score and low engagement in a specific category or workgroup. If you find areas with low patient satisfaction linked to low employee engagement, it is important that you can drill down into the factors that create engagement — such as leadership or supervisory relationship — to identify the engagement drivers that are leading to a low engagement and affecting your patient satisfaction scores. (This will be much easier if you have followed step one and broken down the engagement scores into categories.) Without this level of detail, it becomes hard to know what to do to affect change in the group that is damaging your patient satisfaction scores.
It’s also important to look at both direct staff (nurses and doctors) and indirect staff, because when back-office hospital administrative workers are happier, this has a positive knock-on effect — the less frustration a doctor has to deal with in terms of administrative bottlenecks, for example, the more satisfied they are with their work.
Step 5. Dive deeper
Once you understand which engagement category is impacting patient experience, you need to uncover the root cause of the employee engagement problem. Employee engagement categories will give you a surface view of how satisfied people are with various aspects of their work. To dig deeper into the specific causes, you then need to analyze survey data item by item and support this with input from the local staff and managers. By correlating satisfaction scores with other data, you can gain a clear picture of what is causing the engagement issue.
For example, after reviewing the results of a their employee engagement survey,“I’m over-worked” was identified as a top problem by a Vancouver-based healthcare services provider. The provider then explored why people might feel this way and found the answer in the absenteeism data: some workers were abusing the sick day policy, which left their colleagues stretched too thin.
Step 6. Intervene and take action
Now that you have pinpointed which employee engagement issue is impacting the NPS score, you can build a targeted HR program to address the problem. For example, if feedback about rewards is negative for a work unit that is getting poor performance scores from patients, is there something that can be adjusted in terms of compensation?
Once the new program or policy has been put in place, it is important to continually monitor its effectiveness and adjust accordingly. Continually look at engagement and patient satisfaction data to see if there is any noticeable change.
The Make-or-Break Moment for Healthcare
As Rick Sherwood wrote in this earlier HBR piece, the tie between government reimbursements and patient satisfaction has created a make-or-break moment for financial sustainability: “Losses amounting to millions of dollars for many hospitals and systems that receive half or more of their funding from government reimbursement are possible.”
But fostering a committed, energized workforce is about more than striving to earn an engagement score of 75. This requires HR to dig deep into an ecosystem of data, looking at how to best address the complex drivers of engagement. The more data you have from across your HR transactional systems, the more accurate the analysis, and the better your decisions will be.
Meaningful employee engagement is no longer a “nice-to-have” for hospitals. It is vital for a healthy bottom line.
Get the Outsmart newsletter
You can unsubscribe at any time. For more information, check out Visier's Privacy Statement.


